Cardiac Diary Part 5: ICU—Two Lions and Some Persistent Plastic
It's all done but my time in intensive care came with an unpleasant twist - and some new friends.
Waking up in intensive care is a strange sort of good news. You’re awake—which, given the alternatives, feels like a win. But then you open your eyes properly.
Curtains are everywhere. Not the soft, domestic kind that suggest privacy; these are functional, easy-clean barriers around little islands of crisis. Inside each one is a medical mission control: banks of machines, blinking lights, rolling numbers, and the rhythmic chirping of alarms. At the centre of each lies a person, hovering right on the edge of things.
It doesn’t take long to realise you’re one of them.
Taking stock
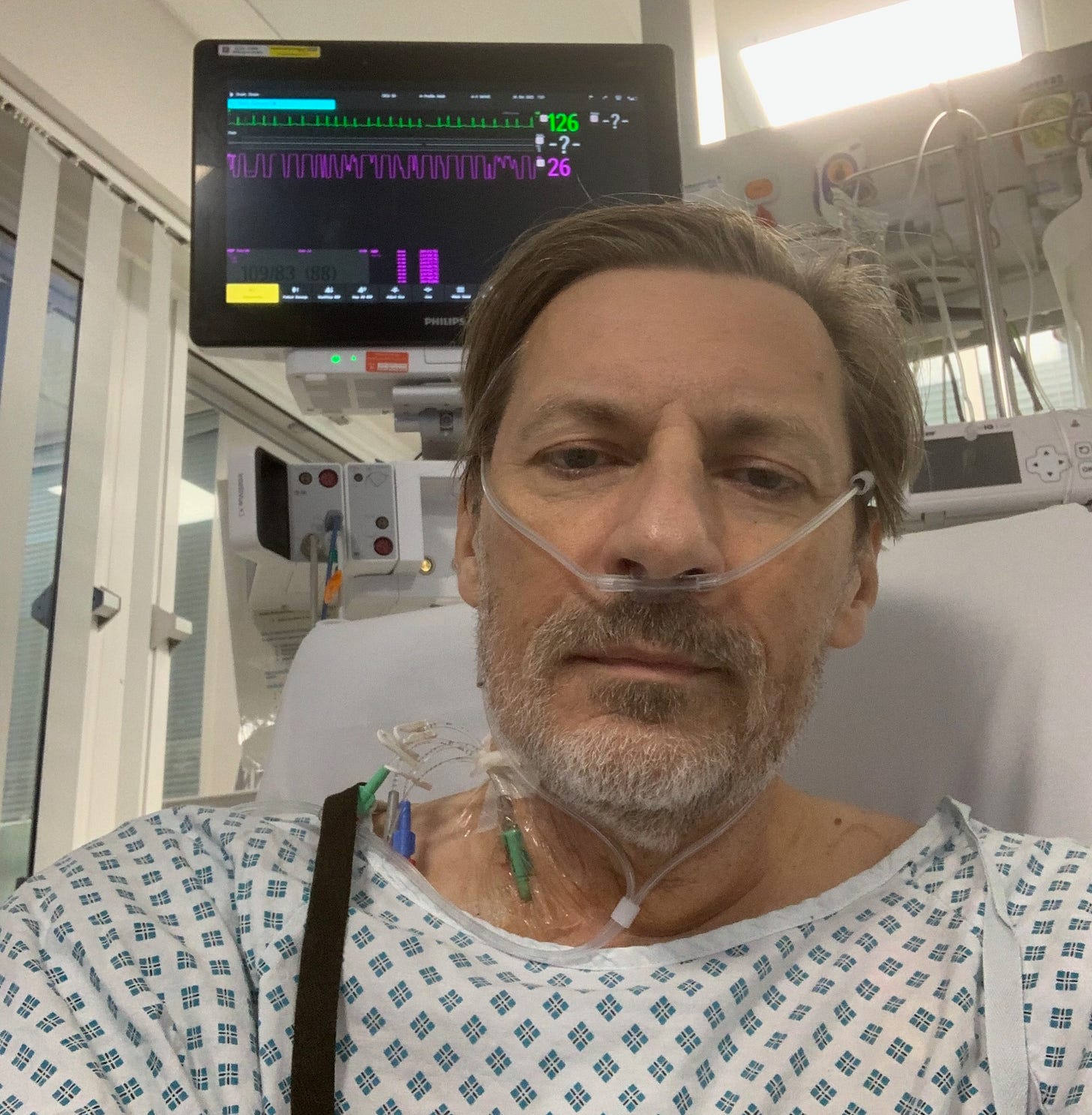
My first conscious act was a groggy, internal stocktake. There was a tube in my neck, and drains in my chest, and wires snaking toward every available limb. Then there was the quiet, unmistakable awareness of a catheter doing its business without once consulting me.
Movement wasn’t so much restricted as it was an improbable ambition. Getting out of bed wasn’t on the agenda; I was less a person and more a tethered satellite. Also, I couldn’t ignore the dressing on my chest—a reminder that something monumental had occurred, even if I was still piecing the details together.
Time as liquid
Trying to construct a timeline was a fool’s errand. I was, to put it mildly, off with the fairies.
Time didn’t move forward so much as it drifted. Days and nights blurred into a cycle governed by “The Routine”: observations, checks, and adjustments.
Oddly, the nights felt the most human. There were long, hushed conversations with whichever nurse had drawn the short straw—quiet chats in the half-light while the machines hummed a mechanical lullaby in the background.
Enter the lions
Then things took a surreal turn. I woke from a nap and found two stone lions at the foot of my bed.
They weren’t enormous, but they weren’t subtle, either. They didn’t do much; they just stood there. Solid. Watchful. Bedside sentinels. I made a quick executive decision not to mention them to the staff. There’s a fine line between “recovering patient” and “extended stay for psychiatric observation,” and I had no interest in crossing it. So, the lions stayed my secret companions.
They came and went. They paced the ward. At one point, the consultant arrived with his entourage—serious faces, important tones, heavy charts. I nodded along politely while, just behind them, my lions wandered about like bored security guards waiting for a shift to end.
A change of pace
After twenty-four hours (it could be longer, it’s all very hazy), the atmosphere shifted.
Before: “Take your time.” After: “Let’s get you out of here.”
I’m told there are “good clinical reasons” for this sudden urgency, but I couldn’t help noticing I had become a unit on a conveyor belt. It was time to move along. Fair enough.
Plastic, be gone
Shortly after, three nurses arrived. That alone felt significant. One nurse is a check-up; three is a “situation.”
“We’re going to remove the drainage tubes,” one said.
I imagined a delicate, calibrated extraction. “Fair enough,” I thought.
“We’ll just pull them out. It might be a bit uncomfortable,” he said, the standard medical code for ‘this is going to hurt.’
I briefly wondered if the other two nurses were there for moral support or to hold me down. I summoned my best brave face. “No problem.”
The first one came out. There is no elegant way to describe the sensation of something being reeled in from deep inside your chest cavity. All I could do was express relief that it was done.
“First one done,” he said brightly.
With all the pain, I’d forgotten—there were two.
The second drain didn’t share its partner’s enthusiasm for departure. There was a pull. Then resistance. Then a look shared between the nurses that suggested we had strayed quite some distance from the script.
A pause. A silent, professional decision made. Pull harder. Pull faster.
Out it came. I gasped—the kind of visceral sound that makes everything else in the world briefly irrelevant. Then came the reveal. The nurse triumphantly held up the tube, only to realise with horror and confusion, the end was missing.
Damage limitation
The atmosphere shifted again. Quiet apologies. A hurried exit. I had just transitioned from “recovering patient” to “incident report.”
Senior figures began to arrive. They didn’t come to fix it; they came to assess. One mentioned—perhaps a touch too casually—that during the pandemic, supply chains had forced them to source “alternative equipment.” You could see the mid-sentence realisation that this was perhaps not the most reassuring trivia to share with a man containing a stray piece of “alternative” plastic.
“Meetings will be had,” I was told. “Enquiries made.”
They didn’t want to be sued. I just wanted the plastic out of my chest.
Back to theatre
A doctor appeared with the air of a man dealing with an inconvenient interruption. He tried a bedside retrieval first—long scissors and a bit of exploratory optimism, which descended into what we Yorkshire people call “broddling about.”
It didn’t work.
“Back to theatre,” he sighed.
Before I could process the defeat of going backward, I was being wheeled away again. They put me to sleep, removed the offending plastic, stitched me back up, and returned me to the ICU to restart the business of recovering.
It was starting to feel like a game of all snakes and no ladders.
The exit
The pace accelerated again after that. With the tubes finally gone, standing became possible. Walking—if you were generous with the definition—followed shortly. The goal was clear: Out.
At some point, I put my Apple Watch back on. It was an attempt at normality that backfired immediately.
Buzz. Ding. “Atrial fibrillation detected.”
Then again. And again. I took it off. There are only so many times a piece of consumer electronics should be allowed to tell you your heart is freestyling. The doctors were calm; it’s common after surgery. It might settle, it might not. Potentially more pills, more procedures. Here we go again.
Eventually, it really was time to leave. In the exit lounge, waiting for my carrier bag of meds to arrive, I got chatting to another patient—a triple bypass. We compared notes in the way survivors do. I mentioned the lions.
He paused, then turned to his wife, looking triumphant. “See? I told you. I saw things.”
His version involved wheelie bins connected by incident tape. We agreed not to analyse that too deeply.
Home
The journey home was slow. Every bump in the road brought a wince of pain, but there was a quiet sense of relief underneath the soreness. Two weeks, from heart attack to discharge. And, all things considered, I’d take stone lions over wheelie bins any day.
This is Part 5 of my Cardiac Diary. In the next post, I’ll write about what happened when I got home and started my recovery and building a ‘new life’. Until next time…
Medical Disclaimer: This article is for general information only and does not constitute medical advice. The needs of every reader are unique; please consult your GP or a qualified healthcare professional before making changes to your diet, exercise routine, or medication. Never ignore professional medical advice because of something you read online.




Stuart, what an amazing story. Glad you survived!! Curious, did you have any scans or tests done before the heart attack. For example CT scan of heart, aka calcium score? And blood work? Or was this a complete surprise? Again, so glad you are here to tell others about your experience.